
Hepatitis C – Diagnostic Serology
Conformément au Règlement de l’Ontario 671/92 de la Loi sur les services en français, les renseignements d’analyses de laboratoire liés à la présente page ne sont offerts qu’en anglais parce qu’ils sont de nature scientifique ou technique et destinés uniquement à l’usage des fournisseurs de soins de santé qualifiés et non aux membres du public.
Background
This page provides serology testing information for hepatitis C virus (HCV) at Public Health Ontario (PHO). For information regarding other testing options, refer to the following PHO webpages:
Updates
- Updated the Acceptance/Rejection Criteria section as follows:
- Cadaveric blood testing services are not available through PHO. Requests can be submitted to Mt. Sinai Hospital Microbiology Laboratory at 416-586-4800 extension 4432.
- Specimens with mismatched information on the label and requisition will be rejected.
Testing Indications
Testing for HCV antibody is indicated for:
- Suspected chronic or acute viral hepatitis
- Unexplained elevated liver function tests (e.g. ALT, AST)
- Screening those at high risk of infection (e.g. intravenous drug users, individuals in correctional facilities, etc.)
- Determining past exposure, needle-stick or occupational exposure
- Epidemiologic investigation (e.g. infection control breach or outbreak situation)
Testing should not be conducted for the investigation of immunity as the presence of HCV antibody does not correlate with protection against HCV.
Acceptance/Rejection Criteria
- Cadaveric blood testing services are not available through PHO. Requests can be submitted to Mt. Sinai Hospital Microbiology Laboratory at 416-586-4800 extension 4432.
- Donor testing is not available through PHO. Specimens from patients being screened as potential donors (e.g. organ, tissue, cells, fertility, etc.) should be referred to a laboratory that performs donor screening assays. Specimens received for donor screening at PHO’s laboratory will be rejected.
- Specimens with mismatched information on the label and requisition will be rejected.
Specimen Requirements
| Test Requested | Required Requisition(s) | Specimen Type | Minimum Volume | Collection Kit |
HCV Serology |
Serum |
1.5 mL serum |
Serum Separator Tube (SST) |
Submission and Collection Notes
Complete all fields of the requisition form, including:
- Test(s) requests and reason for testing
- Patient setting, specimen type and site
- Relevant clinical information
Label the specimen container(s) with the patient’s first and last name, date of collection, and one other unique identifier such as the patient’s health card number or date of birth. For additional information see: Criteria for Acceptance of Patient Specimens. Failure to provide this information may result in rejection or testing delay.
Submit centrifuged serum separator tubes (SST) for serological assays. Centrifugation within 24 hours of collection is optimal for HCV RNA reflex testing.
One full 5 ml SST is required for testing a combination of hepatitis virus markers, HTLV, syphilis and rubella. If a full tube cannot be drawn, submit two tubes.
Refer to Serology Testing – Laboratory Specimen Collection and Submission Instructions for more information.
Do not submit glass tubes.
Limitations
Haemolysed, icteric, lipemic or microbially contaminated serum is not recommended for testing.
Storage and Transport
Place specimen tube in biohazard bag and seal it. Place completed General Test Requisition in the pouch at the front of the biohazard bag.
To avoid delays in testing, ship specimens for testing to PHO immediately after collection or processing. Store specimen tubes at 2-8°C following collection and centrifugation, and ship to PHO’s laboratory on ice packs. If delayed shipping is anticipated, remove serum from clot and store frozen at -20°C or colder, and ship on dry ice.
All clinical specimens must be shipped in accordance to the Transportation of Dangerous Good Act.
Test Frequency and Turnaround Time (TAT)
HCV serology testing is performed daily Monday to Friday.
Turnaround time is up to 3 business days from receipt of the specimen at PHO’s laboratory for non-reactive specimens and up to 6 business days for reactive and indeterminate specimens.
HCV serology testing is performed using two different tests:
- HCV antibody screen: chemiluminescent microparticle immunoassay (CMIA) for the qualitative detection of HCV antibody in human serum. This test does not distinguish between IgG and IgM.
- HCV antibody supplemental test: chemiluminescent immunoassay (CLIA) for qualitative detection of HCV antibody in human serum. This test only detects IgG.
Algorithm
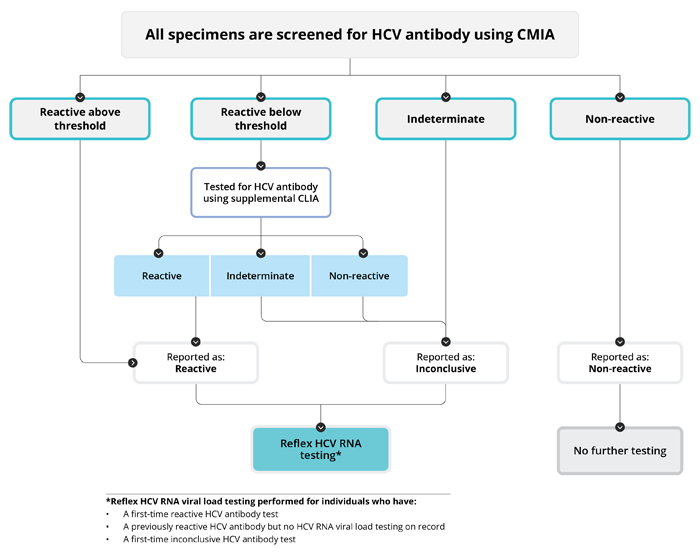
Interpretation
Results should be interpreted in the context of the clinical and exposure history, signs and symptoms of the patient. The table below provides a general overview of possible interpretations. A PHO Microbiologist is available for questions about HCV serology results and interpretations.
|
HCV Antibody Screening Result |
HCV Antibody Supplemental Result |
Possible Interpretations/Comments |
|---|---|---|
|
Non-reactive |
Not tested |
|
|
Indeterminate Reactive Reactive |
Not tested Non-reactive Indeterminate |
|
|
Reactive Reactive |
Reactive Not tested2 |
|
1For infants, testing for HCV RNA earlier than 6 weeks of age is not recommended as assay sensitivity is limited before that age.
2HCV antibody supplemental testing will not be performed if the S/CO value is above PHO’s internally established threshold or if the patient has a history of a reactive HCV antibody result.
Reporting
Results are reported to the physician, authorized health care provider (General O. Reg 45/22, s.18) or submitter as indicated on the requisition.
Specimens that are reactive for HCV antibody are reported to the Medical Officer of Health as per the Ontario Health Protection and Promotion Act. Only first-time reactive HCV antibody results are reported since HCV antibody generally remains detectable for life.
Vous n'avez pas de compte MonSPO? S'inscrire maintenant

